The Utility of Machine Learning in Diagnostic Healthcare
Last Updated on November 1, 2022 by Editorial Team
Author(s): Ina Hanninger
Originally published on Towards AI the World’s Leading AI and Technology News and Media Company. If you are building an AI-related product or service, we invite you to consider becoming an AI sponsor. At Towards AI, we help scale AI and technology startups. Let us help you unleash your technology to the masses.

The last decade has seen a significant rise in the application of AI and machine learning in the field of medicine. However, the ethics, reliability, and suitability of these tools must be carefully considered if it is to replace current traditional approaches. Here I will consider 3 ways in which machine learning may have the potential to benefit healthcare:
1. Redefining and justifying risk thresholds for diseases and disorders
Currently, in diagnosis, many thresholds of risk for disorders such as heart disease tend to be determined with only single variable consideration rather than in a multi-variable sense. For example, when diagnosing heart failure or cardiomyopathy, evidence of an ejection fraction below 40 percent was, for a long time, the gold standard. However, studies have found that about half of all heart failure cases occur with preserved ejection fraction, presenting a grave diagnostic and therapeutic challenge — especially in distinguishing this from other causes of reported symptoms such as difficulty breathing (dyspnoea) [1]. When it comes to pre-symptomatic, at-risk, or early-onset patients of such diseases, even if multiple variables are used, they tend to be arbitrarily combined by clinicians in an independent and associative sense [2].
Presumably, the accuracy of diagnosis would be increased if performed on a case-by-case basis using conditional thresholds across multiple variables — meaning that the threshold for one variable may rely on the value of another. For example, given a patient is 40 years old, male, has a systolic blood pressure of 120 mmHg and a total cholesterol of 4 mmol/L, above what threshold of left ventricular mass would indicate the early onset of heart failure? Or, given this combination of parameter values, what is the patient’s probability of a future onset? Today, even the state-of-the-art AI rule-based decision support used by the NHS in their Electronic Health Record (EHR) system currently lacks this kind of precision [4]
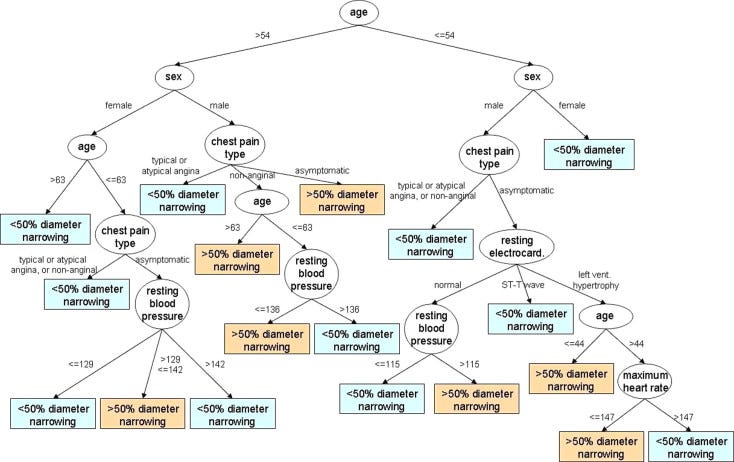
One way this objective could be achieved is through the use of tree-based classification algorithms. Let us theorize that the underlying mechanism of some disorders — aortic stenosis, for example — depends on a complex set of conditional interrelations and logical rules which apply in some cases and not others. For example, we have observed that a high left ventricular mass (hypertrophy) is only a problem if the patient is above a certain age and with a visceral fat mass above a particular value and some other conditions. Tree-based algorithms, such as Decision trees and Random Forests, explicitly learn and model these subgroupings, using conditional decision rules that vary between the branches of its tree, providing different sets of logic for different patients. Simultaneously, facilitates interpretability in the form of feature importances and tree diagrams (such as Figure 1).
It is worth noting that not all machine learning classification algorithms allow for the same type of underlying logic to be inferred. With a singular curve-fitting approach, other discriminant algorithms like SVM, K-nearest neighbors, or logistic regression are not able to learn this type of conditional logic unless pre-programmed.
Over the decades, we have seen various approaches to rule-based systems for medical diagnostics. Starting from MYCIN in the early 1970s, which was used to diagnose blood-borne bacterial infections from multiple variables using a knowledge base of ~600 rules input by experts and an inference engine, to IBM Watson for cancer diagnosis, to the NHS EHR used today; the greatest challenge has been the debate over how best to represent uncertainty, particularly the estimation of a large number of conditional probabilities, and how to deal with the occurrence of conflicting or circular logic in these programmed rules [4].
And even where such rule systems, such as MYCIN, have achieved predictions on par with medical experts, we have not yet seen widespread success or adoption of such systems to set the standard for diagnostic assessment — also due to poor integration with existing clinical systems and concerns about legal responsibility over mispredictions.
2. Developing automatic diagnostic systems with superior accuracy to clinicians
With access to larger amounts of data and further robustness testing, machine learning classifiers may be able to determine the risk and onset of cardiac disorders sooner and more accurately than clinicians can on their own. While (1) looked at how risk thresholds and disease diagnosis could be better defined using machine learning and used as decision support for clinicians, another use case could be on singular tasks where explainability is either less important or irrelevant.

For simple and specific imaging diagnosis, such as detecting the malignancy of pigmented skin lesions, Tschandl et al. (2019) found that classifiers outperformed the judgment of 27 human experts with over a decade of experience, achieving a mean number of correct diagnoses of 25.43 vs. 18.78 (P<0.0001). Similarly, by training an AI on retinal scans DeepMind was able to correctly identify multiple retinal diseases to an accuracy of 94%, surpassing that of top human experts [5]. In other areas, however, limited data and greater complexity behind the factors of influence currently hinder the accuracy and reliability of machine learning compared to humans. And similarly, due to the question of legal culpability over mispredictions, trust in these automatic methods will take greater time to build. For now, it seems wisest to approach any application of machine learning with the philosophy that it should collaborate with and complement human decision-making rather than replace it altogether.
3. Discovering novel insights and theories for medical research
There is often a dichotomy placed between machine learning and traditional statistics in terms of the predictive performance vs. explainability trade-off — that machine learning was designed with greater emphasis on high accuracy prediction while statistics was primarily designed for inferring relationships between variables [6].
However, with developments in machine learning interpretability and explainability tools (e.g., feature importances, SHAP, and Bayesian networks), it is plausible that machine learning has the potential to achieve both high predictive accuracy and insightful explanations. Applied to the context of medical research, one could envisage a future for academia in which mass volumes of patient data are utilized by algorithms to generate causal models which propose new theories and associations between diagnostic variables. In the beginning, these inferences would be ones serving as validations for pre-existing and well-established medical theories, but as confidence grows in the accuracy and wisdom of these algorithms, they may start to be used as the sources of new theories to be studied and supplemented by further patient studies or in-vitro trials.
While such attempts for data mining and knowledge discovery in medicine have existed since the 90s, there are limitations in the methodology behind inferring and proving causality from data, alongside the general challenge of how information should be derived, interpreted, and presented. Quoting the authors of a recent review, unfortunately so, “Biomedical research is drowning in data, yet starving for knowledge.” [7]
References:
[2] Jonathan G. Richens, Ciarán M. Lee & Saurabh Johri. “Improving the accuracy of medical diagnosis with causal machine learning”
[3] C. Hughes “ The representation of uncertainty in medical expert systems”
[4]Thomas Davenport and Ravi Kalakota “The potential for artificial intelligence in healthcare”
[5] https://www.moorfields.nhs.uk/content/breakthrough-ai-technology-improve-care-patients
[6] Danilo Bzdok, Naomi Altman & Martin Krzywinski. “Statistics versus machine learning”
[7] Andreas Holzinger & Igor Jurisica. “Knowledge Discovery and Data Mining in Biomedical Informatics: The Future Is in Integrative, Interactive Machine Learning Solutions”
The Utility of Machine Learning in Diagnostic Healthcare was originally published in Towards AI on Medium, where people are continuing the conversation by highlighting and responding to this story.
Join thousands of data leaders on the AI newsletter. It’s free, we don’t spam, and we never share your email address. Keep up to date with the latest work in AI. From research to projects and ideas. If you are building an AI startup, an AI-related product, or a service, we invite you to consider becoming a sponsor.
Published via Towards AI
Towards AI Academy
We Build Enterprise-Grade AI. We'll Teach You to Master It Too.
15 engineers. 100,000+ students. Towards AI Academy teaches what actually survives production.
Start free — no commitment:
→ 6-Day Agentic AI Engineering Email Guide — one practical lesson per day
→ Agents Architecture Cheatsheet — 3 years of architecture decisions in 6 pages
Our courses:
→ AI Engineering Certification — 90+ lessons from project selection to deployed product. The most comprehensive practical LLM course out there.
→ Agent Engineering Course — Hands on with production agent architectures, memory, routing, and eval frameworks — built from real enterprise engagements.
→ AI for Work — Understand, evaluate, and apply AI for complex work tasks.
Note: Article content contains the views of the contributing authors and not Towards AI.